 Last month, I had the opportunity to give a presentation at the ACHE 2016 Congress on Leadership. This event brings together healthcare executives from across the country to discuss what it means to be a leader, how we can improve in our respective roles, and how we can better ignite inspiration in others in our dynamic healthcare environment.
Last month, I had the opportunity to give a presentation at the ACHE 2016 Congress on Leadership. This event brings together healthcare executives from across the country to discuss what it means to be a leader, how we can improve in our respective roles, and how we can better ignite inspiration in others in our dynamic healthcare environment.
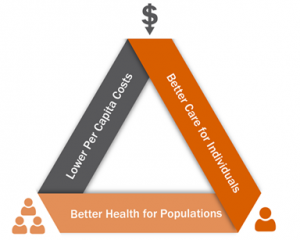
In my session, Dr. Kristin Boehm and I talked about one of the biggest challenges facing hospital execs today: how can we rethink healthcare to realize the benefits of the Institute for Healthcare Improvement’s Triple Aim? The Triple Aim is a framework to change healthcare delivery using three pillars: improving the care experience for the individual patient, improving the health of populations, and reducing the per capita cost of healthcare.
As healthcare execs know, the Affordable Care Act attempts to codify the Triple Aim by transitioning to a value-based reimbursement system in which hospitals and their provider partners assume the risk of caring for populations. This shift from volume to value requires new metrics, new approaches, and unprecedented levels of collaboration between different providers and administrators across the continuum of care. Hospitals need to better understand the outcomes of the healthcare services they are delivering and what the input costs are in order to drive the outcomes they need to maximize reimbursement and minimize penalties.
While alternate payment models require health systems to collaborate with non-acute stakeholders in a new way, they also necessitate a very different level of collaboration within our hospitals. Clinical caregivers and business support departments’like supply chain’must work together closely to evaluate the cost of input selections, the quality of the care provided, and the overall patient outcomes. In fact, I have long argued that supply chain professionals are uniquely positioned to facilitate this collaboration, as they sit at the intersection where individual products converge. Using empirical evidence, the supply chain decision-making process can be shaped to identify and resolve conflicts and create order for competing priorities that can undermine the organization’s ability to deliver the best quality care at the lowest cost.
So how do health system executives facilitate and support a clinically integrated, cost-quality-outcomes (CQO)-focused supply chain?— At ACHE, we emphasized the benefit of implementing physician-led value analysis programs as a means of achieving the Triple Aim. Active involvement of physicians in CQO-based decision-making dramatically increases the likelihood of the successful acceptance and sustainability of product substitutions, conversions, and standardization. It is important to remember that most physicians are trained to be independent decision-makers. The key, of course, is tapping into physicians’ specialized education, experience, and characteristics to champion these efforts.
Beyond empowering physicians with a product evaluation structure using outcomes data, clinically integrated value analysis programs enable ongoing communication with staff at all levels. Most importantly, this behind-the-scenes work should be celebrated. Savings or improved patient outcomes can be reported in internal hospital newsletters and message boards. Scorecards in the OR lounge or physician lunchroom can serve to motivate naturally competitive peers. And process transparency can help build confidence and consensus among affected stakeholders.
While implementing a physician-led value analysis program certainly requires a significant commitment from health-system leaders, open-minded clinicians, and a collaborative supply chain, our message to the ACHE Congress was simple: value analysis is worth the effort. In fact, value analysis is the link that ties a health system’s input and utilization efforts to the Triple Aim. As your hospital continues to strive to achieve the Triple Aim, value analysis is an important, useful tool to connect your clinical leaders and your supply chain professionals as they make decisions that drive cost, quality, and, ultimately, patient outcomes.




Comments are closed.